The kidneys are the primary functional organs of the urinary system, filtering approximately 200 quarts of blood and eliminating waste every day. The kidneys are master regulators that also ensure the body has the proper balance of water and necessary chemicals and minerals, keeping what’s needed and getting rid of what’s not. The kidneys also produce hormones, which support the function of other organs in the body, including hormones that promote the production of healthy red blood cells. The kidneys’ role in regulating the composition of blood and producing hormones affects virtually every part of the body.
Akebia’s purpose is to better the lives of people impacted by kidney disease. We extend our deep appreciation to healthcare providers and we will continue to bring awareness to the importance of kidney health. Watch here for a video sponsored by Akebia that highlights the importance of early diagnosis of chronic kidney disease.
This video is for informational purposes only and is not intended to provide medical advice. Please speak to your healthcare professional for medical advice. The featured healthcare professionals are paid consultants of Akebia Therapeutics, Inc.
37 million
Americans are currently affected by CKD.
Reference
Centers for Disease Control and Prevention. Chronic Kidney Disease in the United States, 2019. Available at: https://www.cdc.gov/kidneydisease/publications-resources/2019-national-facts.html. Accessed: September 3, 2019
Chronic kidney disease (CKD) is characterized by the gradual loss of kidney function and is a serious and life-altering illness that is persistent, progressive, and irreversible. CKD is estimated to affect approximately 37 million adults in the U.S. It is a top-10 leading cause of death in the United States and each year takes more lives than breast cancer or prostate cancer. Having CKD also increases the chances of also having heart disease and stroke.
While CKD is a complex disease with multiple causes and effects, the two main causes are diabetes and high blood pressure. Nearly three-quarters of all CKD cases are associated with diabetes and/or high blood pressure. Approximately one in every three adults with diabetes and one in every five adults with high blood pressure also has CKD.
The progression of CKD is defined by measurement of a patient’s glomerular filtration rate, or GFR. The loss of kidney function is determined by GFR, which is measured by calculating how quickly plasma is cleared of certain substances in the body.
1 in 3
Adults with diabetes also have CKD.
Reference
Centers for Disease Control and Prevention. Chronic Kidney Disease in the United States, 2019. Available at: https://www.cdc.gov/kidneydisease/publications-resources/2019-national-facts.html. Accessed: September 3, 2019.
STAGES OF CHRONIC KIDNEY DISEASE
*GFR is a measure of your kidney function. As kidney disease gets worse, GFR goes down.
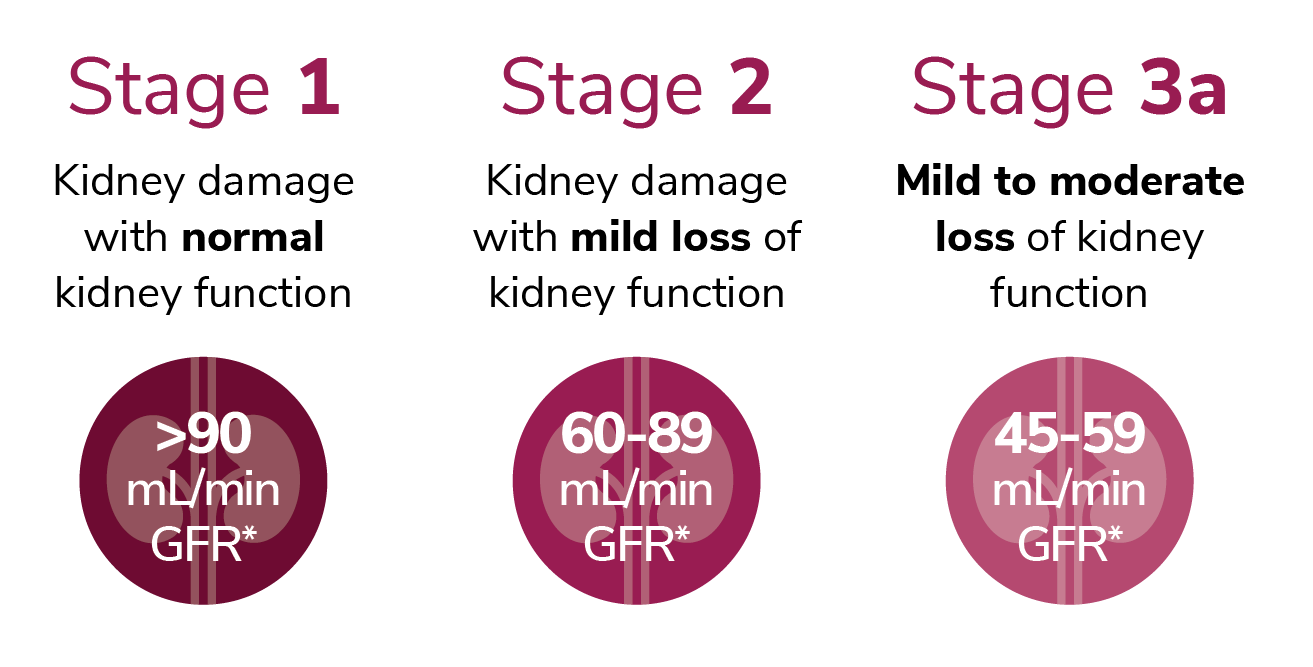
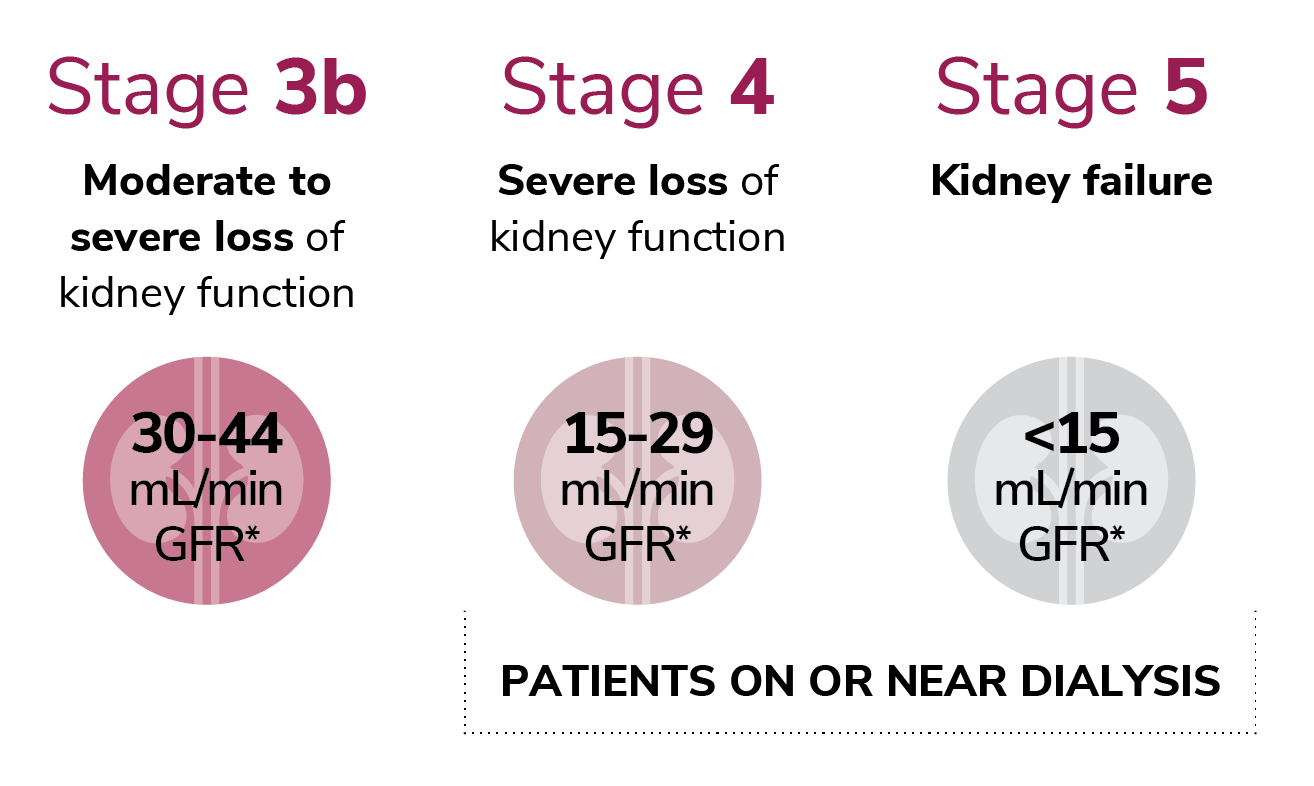
Figure based on: https://www.kidney.org/atoz/content/gfr (accessed on 10/11/19)
As progression occurs through the 5 stages of CKD, an increase in symptoms occurs, and additional health complications can develop as a result of the kidneys’ reduced ability to eliminate waste from the body and produce important hormones. When people with CKD progress to a GFR of less than 15, they have reached Stage 5 and are close to losing or have lost all kidney function. These individuals will typically need to prepare for dialysis, where a machine does the work that the kidneys typically do or prepare for a kidney transplant.
REFERENCES
1. Ogobuiro I, Tuma F. Physiology, Renal [Updated 2019 Feb 10]. StatPearls [Internet]. Treasure Island, FL: StatPearls Publishing; 2019. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538339. Accessed: September 3, 2019.
2. National Institute of Diabetes and Digestive and Kidney Diseases. Chronic Kidney Disease (CKD). Available at: https://www.niddk.nih.gov/health-information/kidney-disease/chronic-kidney-disease-ckd. Accessed: September 3, 2019.
3. National Institute of Diabetes and Digestive and Kidney Diseases. Anemia in Chronic Kidney Disease. Available at: https://www.niddk.nih.gov/health-information/kidney-disease/anemia. Accessed: September 3, 2019.
4. Centers for Disease Control and Prevention. Chronic Kidney Disease in the United States, 2019. Available at: https://www.cdc.gov/kidneydisease/publications-resources/2019-national-facts.html. Accessed: September 3, 2019.
5. National Kidney Foundation. Kidney Disease: The Basics. Available at: https://www.kidney.org/news/newsroom/factsheets/KidneyDiseaseBasics. Accessed: September 3, 2019.
6. United States Renal Data System. 2018 Annual Data Report. Available at: https://www.usrds.org/2018/view/Default.aspx. Accessed: Accessed: September 3, 2019.
7. Baumgarten M, Gehr T. Chronic kidney disease: detection and evaluation. Am Fam Physician 2011;84(10):1138-1148.
8. Stauffer ME, Fan T. Prevalence of Anemia in Chronic Kidney Disease in the United States. PLoS One 2014;9(1):e84943. DOI:10.1371/journal.pone.0084943.
9. Locatelli F, Mazzaferro S, Yee J. Iron Therapy Challenges for the Treatment of Nondialysis CKD Patients. Clin J Am Soc Nephrol 2016;11(7):1269-1280. DOI: 10.2215/CJN.00080116.
10. Fishbane S, Pollack S, Feldman HI, Joffe MM. Iron indices in chronic kidney disease in the National Health and Nutritional Examination Survey 1988-2004. Clin J Am Soc Nephrol 2009;4(1):57-61. DOI: 10.2215/CJN.01670408.
11. Levin A, Tonelli M, Bonventre J, et al. Global Kidney Health 2017 and beyond: a roadmap for closing gaps in care, research, and policy. Lancet 2017;390(10105):1888-1917. DOI:10.1016/S0140-6736(17)30788-2.
BC-0031 (v5.0) 3/22
Hyperphosphatemia
Phosphorus is the second most prevalent mineral in the body and is fundamental to supporting life. Phosphorus gives cells the energy they need to function properly and provides important structural support for bones. Phosphorus is as important to maintaining a healthy body as other minerals, including calcium and iron. Phosphate is naturally found in protein-rich foods.
A major role of the kidneys is to help the body maintain the right amount of phosphorus in the blood. As chronic kidney disease (CKD) progresses, it becomes more difficult for the body to balance phosphorus levels and if too much is retained, a condition called hyperphosphatemia results.
Hyperphosphatemia is a primary hallmark of chronic kidney disease, particularly in people with end-stage renal disease (ESRD) or Stage 5D CKD. The majority of people with end-stage kidney disease who are on dialysis are hyperphosphatemic; almost all people with dialysis-dependent kidney failure experience hyperphosphatemia at some point during the course of their disease. Since high protein intake is recommended for people on dialysis, dietary restriction alone is typically insufficient for controlling phosphate levels.
Anemia in Chronic Kidney Disease
Anemia is a condition in which people don’t have enough healthy red blood cells to carry adequate oxygen to the body’s tissues. Anemia commonly occurs in people with chronic kidney disease (CKD) because of reduced kidney function or low levels of nutrients, such as iron. (See Iron Deficiency Anemia).
One of the key functions of the kidneys is to produce a hormone called erythropoietin (EPO), which is released into the blood to help regulate certain bodily functions, including the production of red blood cells by the bone marrow. As kidney function continues to decline, the kidneys produce less EPO. As a result, less healthy red blood cells are produced, which can commonly result in anemia. The kidneys’ ability to produce EPO worsens as CKD progresses, resulting in worsening anemia.
Anemia due to CKD can not only cause people to feel fatigued, experience headaches, dizziness, or weakness, have trouble concentrating, difficulty breathing, or shortness of breath, but also can result in more serious complications including irregular or unusually fast heart beats, enlargement of the heart, or heart failure.
Iron Deficiency Anemia in Chronic Kidney Disease
Iron deficiency anemia is the most common type of anemia and a common complication of chronic kidney disease (CKD). Anemia is a condition where the body does not have enough healthy red blood cells to deliver adequate oxygen throughout the body. This type of anemia is caused by a lack of iron in the body. Iron deficiency anemia begins to develop in the early stages of CKD and tends to worsen as CKD progresses. The majority of symptoms are mild at first and develop slowly.
More than half of the people living with CKD are iron deficient and don’t produce enough hemoglobin, the component of the red blood cell that carries oxygen.
Iron is an essential mineral for the human body
Iron is the most abundant element on Earth. The iron found in the human body is obtained from the diet and is a critical component of human blood (actually what makes it red). Iron is also used to make hemoglobin, which is a protein needed to make healthy red blood cells that can carry sufficient oxygen throughout the body. When your body does not have enough iron, it will make fewer healthy red blood cells or red blood cells that are too small. People with iron deficiency have low hemoglobin and therefore have less oxygen in their blood.

Akebia Therapeutics, Inc.
245 First Street, Suite 1400
Cambridge, MA 02142
+1 617.871.2098 phone
+1 617.871.2099 fax